Demystifying Andropause: Understanding Male Hormonal Aging and Testosterone Decline

The normal downturn in testosterone levels typically begins in the late 30s/early 40s, and by his 70s, a man’s testosterone levels may have dropped by one-third to one-half.
In this article, we shared how testosterone levels in the male brain slowly decrease with age. In women, this hormonal life change is known as menopause, in men, we call it andropause. In his prime, 95% of male testosterone is made by the testicles in response to signals from the brain. Over the years, the signal gets weaker, and aging testes are less likely to respond. The hormonal downturn typically begins in the late 30s/early 40s, and by his 70s, a man's testosterone levels may have dropped by one-third to one-half. This article will provide more details about andropause, including symptoms, known associated health risks, and natural ways to support this hormonal change.
“Andras'' in Greek means human male and “pause” in Greek a cessation; so literally “andropause” is defined as a syndrome associated with a decrease in sexual satisfaction or a decline in a feeling of general well-being with low levels of testosterone in older men. From a strict medical standpoint andropause is defined as a loss of androgen dominance. Androgens are hormones such as testosterone which are naturally found in higher quantities in the male gender. When a man loses his “androgen dominance” this simply means that he has low testosterone. However, this could also mean that someone could have a “normal” testosterone level but increased estrogen levels and therefore no longer has a dominance of testosterone or other androgens. Some common symptoms and signs that usually come with it include late onset hypogonadism, male climacteric, low T, man-o-pause and Testosterone Deficiency Syndrome.
Andropause is sometimes called ‘male menopause.’ This term is misleading and unhelpful, it implies that men experience a similar hormonal transition as women in middle age. But this isn’t the case. In menopause, the production of the female sex hormones, estrogen and progesterone, drop suddenly. In men, however, there’s a more gradual and less drastic decline in testosterone. Testosterone starts to steadily decline from the age of 30 onwards at a rate of around 1% percent per year. This very gradual decline may develop over several years unlike in women where menopause can develop within months. Often many men chalk up these changes to “ I am just getting older”. They often ignore chronic fatigue or are embarrassed by their lack of interest in sex or sexual performance. It is sad because a simple salivary test is a great tool to detect andropause and it only takes minutes to collect a sample. There are also some blood tests that can be performed as well.
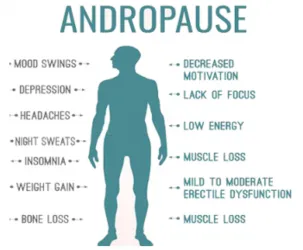
Most men will start to notice symptoms between their late forties to early 50s. A ratio of testosterone to estrogen in normal men is 50:1. With full-blown andropause the ratio is 8:1. Symptoms will begin as soon as testosterone falls below a critical level, regardless of age. Common symptoms of andropause are:
- Decreased libido or sexual desire
- Difficulties with erections
- Low energy or fatigue
- Decreased muscle mass and strength.
- Increase in body fat
- Reduced bone density
- Changes in mood, including irritability, depression, or lack of motivation
- Difficulty concentrating
- Poor sleep
If levels of the hormone estrogen are too high relative to lowering testosterone levels, more serious health concerns can sometimes emerge, such as increased risk for prostate problems and/or cancer, cardiovascular disease, loss of bone density, a rise in cholesterol, and urinary dysfunction. Male bodies need estrogen in smaller amounts to regulate brain and sexual functions in particular. During andropause, "estrogen dominance" can overtake waning testosterone levels, complicating symptoms and raising the risk of prostate cancer.
Five of the main causes of death in men are heart disease, stroke, diabetes, suicide,and Alzheimer’s. It is interesting that many of these diseases can have some of their causation due to a lack of androgen or testosterone dominance. Andropause potentially has huge health effects on men, especially as they age. Most men should be evaluated for this condition before serious health conditions develop.Clinical studies have proven that low testosterone level results are related to the following:
- Increased incidence of Metabolic syndrome/Diabetes ( 33% )
- Increased risk for coronary arterial disease ( 42% ) and atherosclerosis ( 48% )
- Higher incidence of dyslipidemia ( 31% )
- Higher incidence of low mood, depression and sleep disturbances ( 26 %)
- Increased incidence of declining memory ( 21% )
- Decreased libido ( 62 % )
Both male and female hormones originate from a fat called cholesterol. This much maligned fat is vitally important in numerous functions in the human body, and particularly important in sexual and other hormonal production. Those men on cholesterol-reducing medications (statins) should be aware that these medications can potentially reduce testosterone levels. Changes in hormone dominance have huge effects on men and their health. Plainly, there is a complex web of hormones and organs that regulate our health. It is best to balance your body naturally.
If you experience mood-related symptoms, you need to support your emotional health. Ensure that you’re getting between 7 to 9 hours of sleep every night, as sleep is vital for emotional stability. Together, anxiety and sleeplessness exacerbate the effects of each other, perpetuating a negative feedback loop. Regular exercise, meditation, and deep breathing may also support the reduction of stress and anxiety at this time. Eating a diverse, balanced, and mainly ‘whole food’ diet rich in fruit, vegetables, whole grains, healthy fats, and quality protein is critically important for preserving muscle mass, supporting cardiovascular health, maintaining energy levels, and protecting emotional health as you age. Avoiding fast foods, refined carbohydrates, white sugar, partially hydrogenated fats, fried foods, and caffeine is highly recommended. Instead, your diet should contain a lot of natural fiber and lignans from fruits, vegetables, psyllium, flaxseed, apple pectin, etc. Plenty of omega-3 fats from fish, walnuts, flax, and decreased red meat and dairy intake. Maintaining an optimal weight will also support many areas of your well-being, including your sexual health.
Certain herbs and isolated nutrients can also support testosterone production and help with stress and hormonal balance. Below are some of the most researched ones:
- Vitamin D - Adequate vitamin D levels are essential for overall health and hormone regulation. Studies have suggested a link between vitamin D deficiency and low testosterone levels. Sun exposure, fatty fish, and supplementation in the winter months are ways to maintain optimal vitamin D levels.
- Zinc - Zinc is a mineral involved in testosterone synthesis and is crucial for maintaining reproductive health. Zinc supplementation has been found to increase testosterone levels and improve symptoms of andropause. Oysters, beef, pumpkin seeds, and legumes are excellent dietary sources of zinc
- Ashwagandha - Ashwagandha is an adaptogenic herb known for its stress-reducing properties. It may help alleviate symptoms of andropause, such as anxiety, fatigue, and reduced libido.
- Saw palmetto - Saw palmetto is a popular herbal remedy that can support prostate health and alleviate urinary symptoms associated with andropause. It may help reduce prostate enlargement and improve urinary flow.
- Korean red ginseng - Korean red ginseng is a herb known for its potential benefits on sexual health and vitality. It may help improve erectile function, libido, and overall energy levels.
As we were researching this topic, we found a huge discrepancy in the information shared prior to 2005 versus post that time frame. The earlier articles suggested that there was a great deal of medical debate about andropause, but most agreed that there was no doubt that older men can be severely impacted by low testosterone levels. They also noted that there were no scientific clinical trials yet to show that giving men extra testosterone has any effect. One article noted that studies of women taking estrogen replacement showed that 30 to 40 per cent of the benefits reported were from placebos, and that testosterone replacement would soon be as normalas hormone replacement therapy for women. This would occur because doctors and the public won't be able to withstand the drug companies' marketing onslaught for much longer. It was estimated that between five to 10 years, andropause would be officially categorized as a medical condition resulting in massive investments in its treatment.
So what do ALL of the articles from approximately 2014 on say about andropause? All of them say that if a man is having any of the symptoms, he can cure it by using hormone replacement. Once again, we see the pharmaceuticals cashing in on a process that naturally occurs with aging. They cash in on the public’s attitudes toward a population of aging men in a culture obsessed with youth. Men want to remain young longer, so the drug companies see the possibility of enormous profits. Pfizer set the trend with Viagra, and popular books bring the idea of the male menopause to the attention of huge numbers of men.
Our question to all of you is, when are we going to stop looking for the fountain of youth and realize that it can not be found in synthetic drugs? The answers lie within each of us; we just have to be brave enough to find them.


